Fractures
Don Fitz-Ritson, DC, FCCPOR(C), and Stephanie Kim, BSc, DC
Fractures are a common injury in any sport, Early research suggests the application of low-level laser therapy may help accelerate the healing process.
Low-level laser energy has a non-thermal , bio-stimulative effect on biological tissues. The therapeutic application of low-level laser energy, frequently known as (LLLT), produces beneficial clinical effects in the treatment of musculoskeletal and soft tissue conditions.
LLLT is non-invasive and avoids the potential side effects of drug therapy. More specifically, LLLT delivers light energy - photons to targeted tissue, penetrating the layers of skin to reach internal tissues to produce a specific, non-thermal photochemical effect at the cellular level. (1)
Some of the known effects of LLLT include the enhancement of ATP production, which acts as the trigger for the bio-stimulating effect (2), improved microcirculation and bone regeneration. (3)
LLLT devices apply light energy at a wavelength in the near-to mid-infrared range, along with specific parameters that govern the Joules dosage, frequency, time, duty cycle and cadence of light energy being applied. For example, known LLLT protocols for treating specific pain symptoms involve precise settings that not only allow light energy - photons - to enter the tissue, but the protocol parameters interact with the known physiology of the body for pain relief and proper healing of the tissue. (3)
Currently, methods for treating bone fractures, such as setting the bone and casting, are limited by the duration of the body's healing process. No known methods currently exist to accelerate this healing process. This is particularly a problem for the elderly and others patients with fragile bones and slow healing processes. However, because of the enhancing effect of LLLT on microcirculation and bone regeneration, it is likely to aid in the treatment of bone fracture by accelerating the healing process.
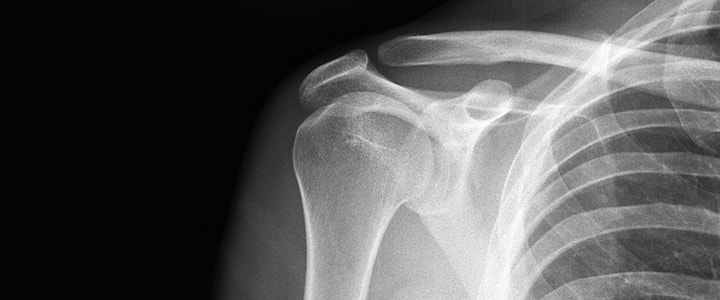
A 52-year-old female presented to our centre with a left humerus fracture. She said she in-line skating down a ramp at a fast speed, lost control and hit her left shoulder hard against a rail.
X-rays of her left shoulder showed a closed,comminuted, spiral fracture involving the greater tubercle and surgical neck of the humerus. The orthopedic surgeon decided it was a high risk to perform surgery due to the nature of the fracture, and palced her arm in a sling and released her.
Examination of her left shoulder revealed a large deep purple and green ecchymosis over her left anterior, posterior and lateral shoulder down to her left elbow. General swelling and heating was noted in the left shoulder and upper arm. The patient reported a dull, achy pain in the shoulder, occasionally extending to her forearm. She rated her pain as nine out of 10 on the pain scale. She also reported a stiff neck and associated headache. Neurological examination and circulation of ther upper extremities were within the normal range.
A pulsed laser using a specific protocol was applied over her left shoulder, forearm and neck for 10 treatments on alternate days. The patient visited the orthopedics surgeon and a second set of X-rays indicated new bone formation. General swelling/ecchymosis/pain was reduced by 80 percent. The patient began physiotherapy starting with range of motion exercises.
After 19 treatments, a third set of X-rays of the humerus showed improved healing on the lateral side and new bone formation on the medial aspect. There was also a complete resolution of ecchymosis and swelling and she reported no pain. The patient progressed to active and resisted muscle training and was discharged from laser therapy.
Laser Research
Luger (4) stated that low-power laser irradiation (LPLI) has been found to have a positive effect on bone fracture healing in animal models, based on morphogenic, biochemical, roentgenographic, and electron microscopic measurements. He then validated his claim experimentally by breaking the tibia of rats, and treating the injury with LPLI (HeNe Laser 632.8nm, 35mW). This was applied transcutaneously over 30 minutes to the area of the fracture, every day for 14 days. After four weeks, the tibia was removed and tested at the tension up to failure. The maximal load at failure and the structural stiffness of the tibia were found to be elevated significantly in the irradiated group ( P=.014 and P=.0023 , respectively), wheras the extension maximal load was reduced (P=.015)
Silva Junior (5) showed that stimulating broken bones for three or 12 sessions with LLLT caused an increase in bone repair and early bone healing.
In a study to evaluate whether low-power laser bio-stimulation of the osteochondral lesions of the knee could by itseld reduce healing time, Morrone (6) showed that with one treatment for 10 minutes, LLLT of th eosteochrondal lesions caused faster healing of the lesion at week two (p=0.043) and an overall improvement in cellurlar morphology(p=0.044)., while a more regular aspect of the osteocartilaginour tissue was observed at week 12(p=0.004).
The effect of low-nergy laser (He-Ne) irradiation on repairing bone in cortical part of the tibia of rats was investigated using biochemical and radioactive labeling methods. A fixed round hole was created in the lateral aspect of the tibia and the newly formed tissue was collected from the gap in the cortical bone to ascertain normal healing response rate. Alkaline phosphatase (ALP) and calcium progressively accumulated at the site of injury, peaking at nine and 13 days post-injury, respectively. Direct irradiation of the whole injury with He-Ne laser, on days five and six post-injury, altered osteoblastic actively at the injured site as reflected by ALP activity.
The laser irradiation also caused a significant increase (approximately two-fold) in calcium accumulation at the site of injury for nine to 18 days post-injury. The rate of calcium deposition, measured by radioactive calcium, was significantly higher (approximately two- folder) in the laser-irradiated rats as compared with controls. The conclusion was that the process of bone repair in a hole created in the rat tibia is markedly enhanced by direct He-Ne laser irradiation of the injured site at the optimal energy level and time post-injury. (7)
Similar results were also obtained when either osteochondral lesions were applied to the animal knees(8), observing the natural growth of bones. (9) or with dental pulp, (10) where results suggested that formation of calcified nodules in human dental pulp cells, as well as in ALP activity,the production of collagen and osteocalcin were enhanced by laser irradiation.
Does the type of laser used affect the rate of bone formation? Ninomiya, 11, provided data that demonstrated the number of pulses, rather than the intensity of the laser irradiation, affects bone formation. His study indicated that high-intensity pulsed laser irradiation accelerates bone formation in the metaphysic. This bone formation induced by high-intensity pulsed laser irradiation might be due to the laser-induced pressure waves.
Ueda, 12, showed that both continuous and pulsed laser irradiation significantly stimulated cellular proliferation, bone nodule formation, ALP activity, and ALP gene expression, as compared with the non-irradiation group. Notably, the pulsed laser markedly stimulated these factors, when compared with the continuous laser. He concluded that it is most likely that pulse frequency is an important factoraffecting biological responses in bone formation.
Summary
From the case history results, the laser and protocols applied and the references cited, there is evidence suggesting the beneficial effects of LLLT for the treatment of bone fractures. Further research is necessary to identify at what point it is most advantageous to initiate the LLLT, what frequency is best (daily, every second day, once/week), the length of time for the therapy, (five, 10 or 30 minutes).
These factors, along with specific parameters of the lasers, all need further study so that treatment will work in harmony with the physiology of the body and bone regeneration for optimal results.
References:
- Basford J., Laser Therapy: Scientific Basis and Clinical Role. Orthopedics 1933; 16: 541-547.
- Karu T. Molecular mechanism of the therapeutic effect of low-intensity laser irradiation. Lasers in the Life Sciences 1988; 2:53-74.
- Turner J, Hode L, editors. Low Level Laser Therapy: Clinical Practice and Scientific Background. Prima Book Publishers 1999, 87-89.
- Luger E, Rochkind S, Wollman Y,et,al. Effect of low-power laser irradiation on the mechanical properties of bone fracture healing in rats. Lasers Surg Med 1998: 22(2):97-102.
- Silva Junior A, Pinheiro A, Oliveira M, et, al. Computerized morphometric assessment of the effect of low-level laser therapy on bone repair: an experimental animal study. J CLin Laser Med Surg 2002: Apr;20(2):83-7.
- Morrone G, Guzzardella G, Torricelli P, et, al. Osteochondral lesion repair of the knee in the rabbit after low-power diode Ga-Al-As laser biostimulation: an experimental study. Artif Cells Blood Substit Immobil Biotechnol 2000 Jul; 28(4):321-36.
- Yaakobi T, Maltz L, Oron U. Promotion of bone repair in the cortical bone of the tibia in rats by low-energy laser (He-Ne) irradiation. Calcif Tissue Int. 1996 Oct; 59(4):297-300.
- Guzzarlella G, Tigani D, Torricelli P, et, al, Low-pwer diode laser stimulation of surgical osteochondral defects: results after 24 weeks. Artif Cells Bloods Substit Immobil Biotechnol 2001 May: 29(3): 235-44.
- Mavrich V Features of growth and chemical compostion of various skeletal bone s of albino rats as affected by X-ray and laser irradiation. MOrfologiia 1999; 116(4):57-60.
- Ohbayashi E, Matsushima K, Hosoya S, et, al, Stimulatory effect of laser irradiation on calcified nodule formation in human dental pulp fibroblasts. J Endod. 1999; Jan: 25(1):30-3.
- Ninomiya T, Miyamoto Y, Ito T, et, al. High-intensity pulsed laser irradiation accelerates bone for formation in metaphyseal trabecular bone in rat femur. J Bone Miner Metab. 2003; 21(2):67-73.
- Ueda Y, Shimizu N, Pulse irradiation of low-power laser stimulates bone nodule formation. J Oral Sci. 2001 Mar; 43(1) 55-60.
Chronic Pain Relief
